SPECT/CT advances routine oral cancer assessment
May 18, 2017 — With the addition of SPECT/CT, clinicians can find previously undetected sentinel lymph nodes in patients with early-stage oral cancer, according to a study published in the June issue of the European Journal of Nuclear Medicine and Molecular Imaging.
An article by Wayne Forrest
from Auntminnie.com
Given the prowess of the hybrid modality, Dutch researchers are recommending the addition of SPECT/CT to planar lymphoscintigraphy to identify more positive sentinel lymph nodes and give surgeons a better guide to biopsies and more effective treatment.
“In a multidisciplinary setting, both imaging modalities were separately investigated, and in 22% of the patients, additional sentinel lymph nodes were found on SPECT/CT imaging,” noted lead author Dr. Inne J. den Toom and colleagues from VU University Medical Center in Amsterdam. “In 20% of the sentinel lymph node-positive patients, the positive sentinel lymph nodes had been identified only with SPECT/CT.”
Biopsy shortcomings
Sentinel lymph node biopsy can be an effective method for the detection of early-stage oral cancer, but the procedure also has been shown to have limited accuracy among patients with floor-of-mouth tumors (EJNMMI, June 2017, Vol. 44:6, pp. 998-1004).
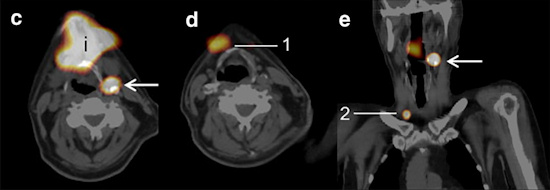
SPECT/CT (c, d, e) shows additional sentinel lymph nodes (arrows) on the tongue, with planar lymphoscintigraphy indicating postinjection spot (i). Due to the high amount of tracer uptake on SPECT/CT, exploration with the gamma probe was performed during surgery, during which three sentinel lymph nodes were identified (1, 2). Images courtesy of EJNMMI.
At VU University Medical Center, clinicians perform dynamic and static planar lymphoscintigraphy using a technetium-labeled (Tc-99m) tracer to investigate sentinel lymph nodes. SPECT/CT also is part of the routine protocol to evaluate patients with suspected early-stage oral cancer. However, until this paper, den Toom and colleagues contend that no large-scale study has been conducted to determine what additional information SPECT/CT can provide in these cases.
The researchers enrolled 66 consecutive patients with early-stage oral cancer (T1-T2) into the study between June 2011 and January 2014. The subjects also presented with clinically negative results (cN0) for neck cancer.
All patients underwent sentinel lymph node biopsies through a two-day protocol that included injections of technetium-labeled nanocolloidal albumin (Nanocoll, GE Healthcare) at the closest proximity of the primary tumor. Planar lymphoscintigraphy was started directly after injection of the tracer. Planar and SPECT images were acquired with a SPECT/CT gamma camera (Siemens Healthineers). The addition of SPECT/CT to planar images was retrospectively analyzed for the number of additional sentinel lymph nodes, for more precise localization of sentinel lymph nodes.
A nuclear physician, head and neck surgeon, and an investigator with considerable experience in sentinel lymph node biopsies and early-stage oral cancer then evaluated the images. The group first read the planar lymphoscintigraphic images alone, then compared the planar results with the SPECT/CT to determine additional information gleaned from the hybrid modality.
Image analyses
In reviewing the results, the researchers identified sentinel lymph nodes in 65 (98%) of the 66 patients. They found at least one positive sentinel lymph node in 10 patients (15%), while the discovery of additional metastases upstaged the cancer diagnoses in two patients (3%).
SPECT/CT detected 15 additional sentinel lymph nodes in 14 patients (22%). The new discoveries were related to other sentinel lymph nodes that had been found in the same, adjacent, and nonadjacent levels or on the other side of the neck. In two (14%) of these patients, positive sentinel lymph node identification was due to the addition of SPECT/CT. In addition, metastases were found in two sentinel lymph nodes (13%).
SPECT/CT also was instrumental in discerning masses among the 66 patients. In five cases (8%) in which planar lymphoscintigrams leaned toward diagnoses of sentinel lymph nodes, SPECT/CT reversed the finding to nonsentinel lymph nodes. Also, there were four false-negative sentinel lymph node biopsy procedures in this cohort.
“In 20% of the patients with at least one positive sentinel lymph node, the only positive sentinel lymph node was detected due to the addition of SPECT/CT,” the authors wrote. “Moreover, SPECT/CT provides better topographical orientation for the surgeon preoperatively.”
They added that in a multidisciplinary setting, both imaging modalities were separately investigated, and in 22% of the patients, additional sentinel lymph nodes were found on SPECT/CT. This resulted in an upstaging rate of 3% in all patients, especially in patients with floor-of-mouth tumors.
The team also emphasized that SPECT/CT provided enhanced preoperative anatomical information for surgeons for all 66 patients. The additional data were most important for the two patients who had their early-stage oral cancer upgraded.
“Due to the better topographical orientation, the anatomical levels of the sentinel lymph nodes had been changed in 28% of the patients and better delineation against surrounding tissues could be done,” the authors noted.
http://www.auntminnieeurope.com/index.aspx?Sec=sup&Sub=mol&Pag=dis&ItemId=614476
